Snoring is often dismissed as a minor issue. However, it is actually a specific physiological phenomenon: an increase in resistance in the upper airways during sleep.
Beyond the nighttime noise, snoring indicates a respiratory imbalance that can affect sleep quality… and sometimes lead to more severe conditions.
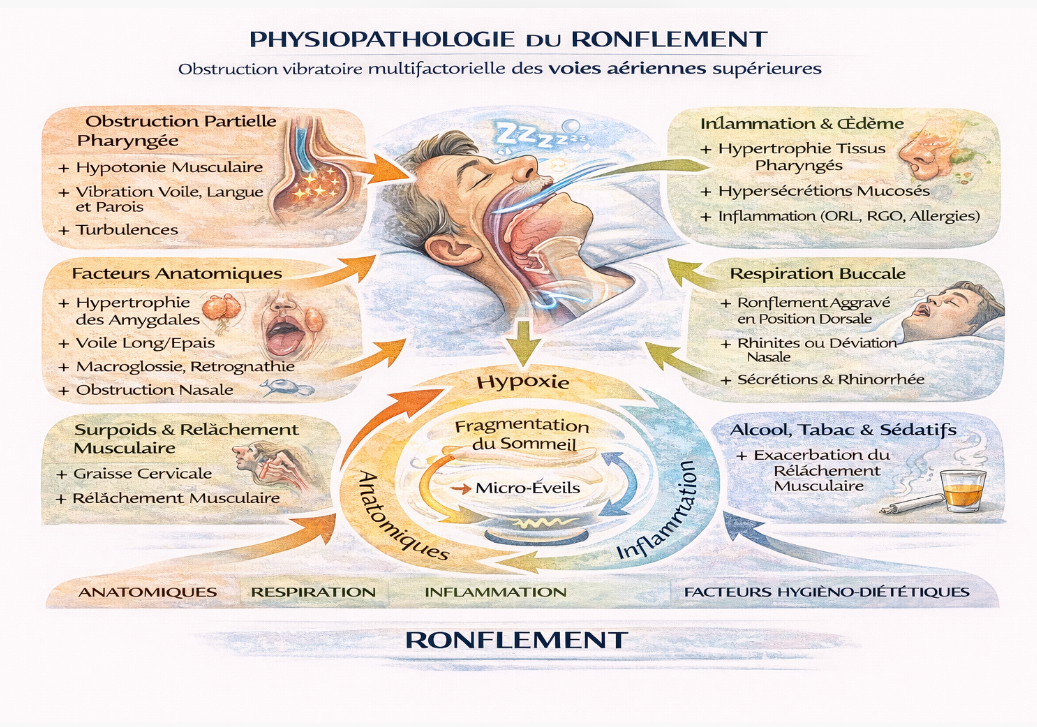
1. The mechanism of snoring: partial airway obstruction
Snoring occurs when the upper airways partially narrow, primarily at:
the soft palate
the uvula
the base of the tongue
the pharyngeal walls
When inhaled air flows through a narrowed space, the airflow becomes turbulent. This turbulence causes the soft tissues to vibrate—which is what generates the characteristic sound of snoring.
2. The role of sleep and muscle relaxation
During sleep—particularly during REM sleep—muscle tone naturally decreases:
The muscles that widen the pharynx relax
The tissues become more supple
The airway diameter narrows
This is a physiological phenomenon.
However, when combined with other factors (inflammation, excess weight, nasal obstruction), the risk of snoring increases significantly.
3. Anatomical factors that contribute to snoring
Certain anatomical features increase the likelihood of snoring:
These factors mechanically reduce the diameter of the airways and amplify vibrations.
4. Nasal breathing, inflammation, and secretions
Impaired nasal breathing (chronic rhinitis, allergies, gastroesophageal reflux, sinusitis) leads to:
Chronic inflammation of the mucous membranes causes:
The tissues then become more vibrating and more sensitive to airflow.
5. Alcohol, stress, and aggravating factors
Certain behavioral factors increase airway collapsibility:
Alcohol
Sedatives
Chronic fatigue
Stress
Lack of rest
They increase nighttime muscle relaxation and promote snoring.
6. Simple snoring or a warning sign?
Snoring is part of a pathophysiological continuum:
Simple snoring
Increased airway resistance syndrome
Obstructive sleep apnea-hypopnea syndrome (OSAHS)
Chronic, loud snoring, or snoring accompanied by pauses in breathing, daytime sleepiness, or morning headaches should be evaluated by a healthcare professional.