Heartburn, often associated with gastroesophageal reflux disease (GERD), is caused by the abnormal backflow of stomach contents into the esophagus and sometimes into the upper airways.
It’s not just heartburn.
GERD can also cause:
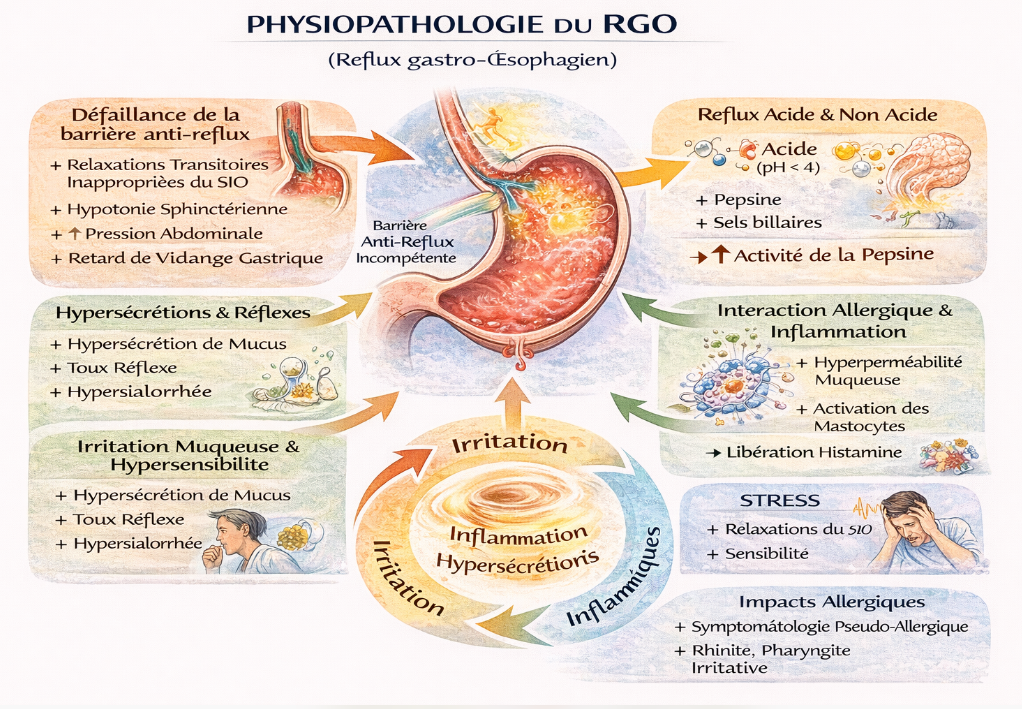
Understanding its pathophysiology allows for more targeted treatment.
1. Why does reflux occur?
Reflux occurs primarily due to a dysfunction of the lower esophageal sphincter (LES).
This sphincter acts as a valve between the stomach and the esophagus.
When it becomes incompetent, several mechanisms promote acid reflux:
Gastric contents (acid, pepsin, and sometimes bile) then flow back up into the esophagus.
2. Acid reflux… but not only that
We distinguish between:
Even without significant acidity, pepsin remains biologically active and can irritate the ENT mucous membranes.
👉 This is why some patients continue to experience symptoms despite antacid treatments.
3. Mucosal irritation and hypersensitivity
Repeated exposure to reflux leads to:
Even small amounts of reflux can then cause:
We often refer to laryngopharyngeal reflux when the symptoms are primarily ENT-related.
4. Chronic inflammation and mucus production
Repeated irritation triggers an inflammatory response:
In response, the body produces more mucus to protect itself.
➡️ This mucus can sometimes become excessive and leads to:
Throat clearing
A feeling of congestion
Reflex cough
This inflammatory cycle explains why symptoms become chronic.
5. GERD, allergies, and stress: a common interaction
GERD does not occur in isolation.
It interacts with:
Stress increases relaxation of the esophageal sphincter and heightens symptom perception.
Allergies can increase mucosal permeability and exacerbate local inflammation.
It is therefore a complex functional and inflammatory disorder.